Robust Polymers Are Key to Advancing Robotic Surgery
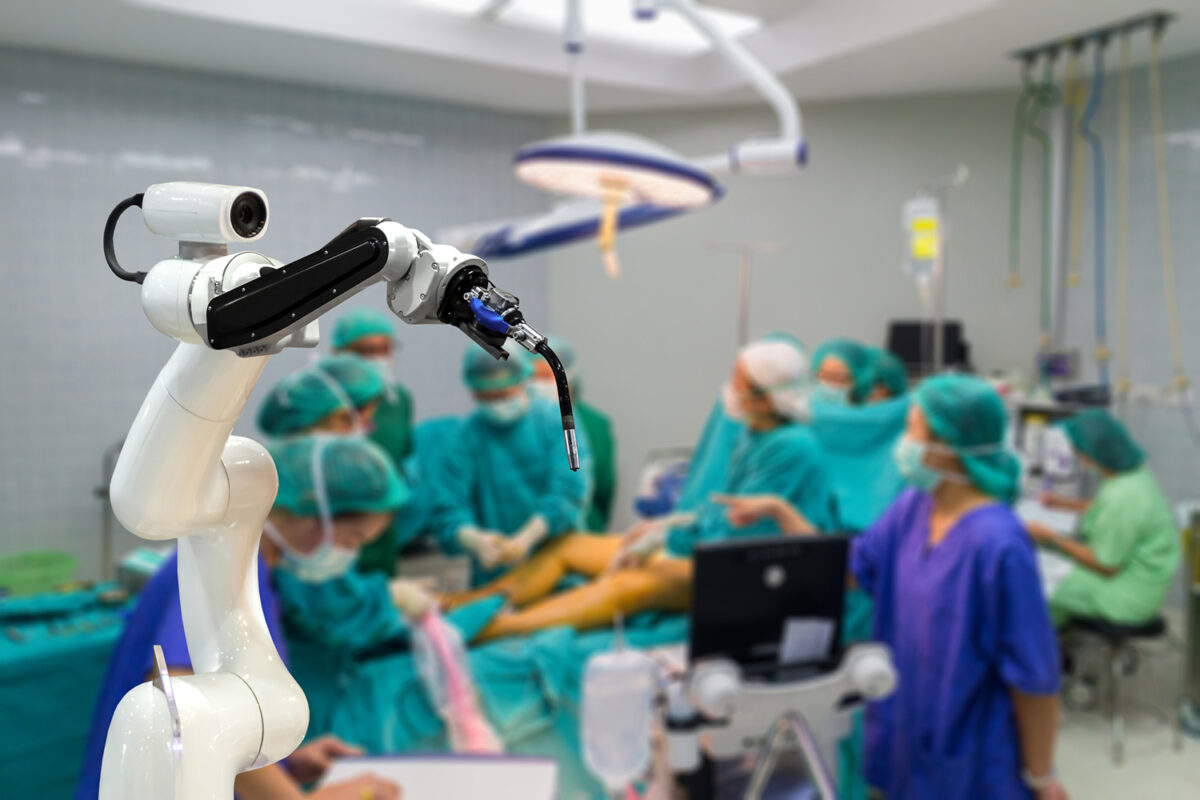
Work is underway to combine plastics and electronics to further medical capabilities
Second of a three-part report
The growing electronification and robotification of medical technology offer opportunities for the use of plastics in the high-precision robotics that will increasingly be developed for these exacting and automation-rich applications.
Current and future plastics in medical devices will work seamlessly with surgical robots and the tools they use; precisely guide, at times with nano-scale accuracy, robotic instruments in extraordinarily delicate invasive procedures; and withstand multiple harsh sterilization procedures since most robotic devices will be reused.
Plastics will need to be extremely robust to contain the advanced and progressively smaller electronics that power and guide robots in procedures, said Neal Walters, a partner at the global management consulting firm Kearney. Walters has analyzed this market and the manufacturing and supply issues it presents for almost 20 years. He recently co-authored a Kearney paper titled, “The great global supply chain reset is here. Are you ready to regenerate?”
In the first part (Sept. 28) of this series on electrification and robotification of medical technology, Walters highlighted the new world of device manufacturing and use that relies on high-tech electronics, robotic surgery and remote monitoring of implanted sensors to promote patient health. In this post he provides a view of what surgical robots can routinely accomplish with advanced electronics and high-performance polymers.
Precision Surgery Needs Promote Robot Use
Robotic surgeries are so precise, he remarked, that they are already used in sensitive procedures, where probes must accurately penetrate extremely small, almost microscopic openings in organs for biopsies and repair.
“These surgeries allow doctors to robotically insert probes and implants with high precision,” Walters said. “Today, when a doctor does a biopsy, there’s always some risk of missing a diseased area. With robots that have cameras and scalpels, you know precisely that you’re getting the right tissue.” If, in the procedure, tissue tests on site as malignant, action could eventually begin to immediately treat the tumor and only the tumor, he advised.
This capability is 2 to 5 years away, Walters reckoned, and may not by then involve traditional therapies such as chemo or radiation. “This really has the potential to revolutionize early detection and treatment of some malignancies,” he said.
Might a robot that conducted a biopsy be equipped in the near future with instruments that immediately test a sample for cancer and begin treatment of the disease on the spot?
“There will always be an ability as artificial intelligence grows to do fairly accurate pre-diagnoses. But the final diagnosis, at least in the near term, is likely to still require a lab. Robots today have integrated cameras and cutting tools. In 2 to 5 years, doctors can start treating a tumor directly. Imagine beginning treatment minutes after a biopsy as opposed to waiting days or weeks.”
A Better Way to Do Invasive Procedures
The accuracy of robotic surgery would change procedures. Those that require precise navigation of very small spaces in the body, including the lungs, heart and brain, he said, would be candidates for robotic surgery. And this will inevitably disrupt the economic model of medical research and practice. “A lot of research today focuses on which developments will have the biggest impact for the most patients. The future will be one in which the biggest impact for every patient and the economic impact of this will have to be considered.”
Plastics will need to have the dimensional stability and durability to accurately guide and place devices in surgeries. Consider a replacement knee. “There will be micro sensors in the knee that detect motion and transmit these data to a cloud-based retrieval system. Small and robust will be key for the sensors,” he said. “If it’s in a knee joint, you don’t want an invasive procedure to correct a mistake or add a better sensor—you’d never put a patient through an invasive procedure to replace a sensor. These electronics will need to be robust and will be easier to integrate into plastics than metal. They must meet the expected lifetime of the device—10 to 20 years with limited chance for replacement. This requires micro sensors. For plastics, the challenge will be how they are incorporated into a plastic device, so they are safe, secure and robust.”
But once implanted, Walters said, the data will flow about how a patient reacts to the implant and how well rehabilitation goes. “Where historically a knee would be just the physical implant, the device industry is working toward cases where sensors allow doctors to monitor physical recovery in real time. This is a major benefit of remote sensing and implantation of sensors.
In the concluding post, we will look at trends and concerns that affect the manufacturing of these advanced medical devices. Read part one here.
